Covid Deaths are Down
Weekly total U.S. Deaths from Covid-19 are down for the 9th consecutive week in a row:
Deaths — Week Ending
18,437 — April 18
15,242 — April 25
13,188 — May 2
12,593 — May 9
10,076 — May 16
8,570 — May 23
6,874 — May 30
6,539 — June 6
5,431 — June 13
4,453 — June 20
However, weekly total U.S. new cases of Covid-19 are up this past week over last week by 34,674 extra new cases. For the same period as the weekly deaths above, new cases were down every week for the first six consecutive weeks, then they were up and down, successively.
Interpretation: More persons are getting sick, but fewer are dying. When cases are up, but deaths are down, it could mean that hospitals and doctors are getting better at treating the disease. This seems to be the case, so it is at least part of the reason for the lower death rate.
However, an alternate interpretation is that more persons are getting outside, in warm weather, with skin exposed to sun. This produces vitamin D, which has been shown by at least a dozen studies, discussed here and here, to have beneficial effects in fighting Covid-19. Higher levels of vitamin D in the blood reduce risk of a severe case of Covid-19, and reduce risk of death from the disease. Some infectious diseases are seasonal; they are cyclic, for this very reason. A couple of recent studies [1, 2] proposed that Covid-19 is also seasonal. So we may simply be entering the more favorable season for this disease. If so, then winter will be worse, far worse.
Vitamin D
A new study found that untreated vitamin D deficiency was associated with a 77% increase in likelihood of Covid-19 infection. Persons with sufficient vitamin D were 56% less likely to become infected with Covid-19. [3] The evidence continues to accumulate that vitamin D has substantial benefits against Covid-19, reducing risk of infection itself, reducing risk of a severe case of the disease, and reducing risk of death.
At this point, vitamin D should be recommended to every adult.
“To reduce the risk of infection, it is recommended that people at risk of influenza and/or COVID-19 consider taking 10,000 IU/d of vitamin D3 for a few weeks to rapidly raise 25(OH)D concentrations, followed by 5000 IU/d. The goal should be to raise 25(OH)D concentrations above 40–60 ng/mL (100–150 nmol/L). For treatment of people who become infected with COVID-19, higher vitamin D3 doses might be useful.” [4]
The number of lives that could be saved is monumental. In addition, fewer severe cases and fewer infections means a vast reduction in suffering as well. For those persons who cannot afford or obtain vitamin D, such as the millions of persons in poverty in the developing world, exposing skin to sunlight provides as much vitamin D as supplementation.
Vitamin K
Critically ill Covid-19 patients often experience severe thrombosis, a blood clotting in the veins or arteries. The most common type (87%) was pulmonary thrombosis (blood clots in the arteries of the lungs) [5]. Other types of thrombosis occurred in the deep veins or in the arteries. “Patients diagnosed with thrombotic complications” had more than 5 times the risk of all-cause death [5]. Therefore, avoiding thrombosis is an important goal in treating Covid-19 patients. However, therapeutic anticoagulation had no effect on risk of death [5], thereby indicating that, although anticoagulation is obviously a necessary treatment, another medication is needed to prevent coagulation in the first place.
A study of vitamin K levels and coagulation (clotting/thrombosis) found that Covid-19 patients had low levels of vitamin K compared to other (non-Covid-19) patients, and low levels of vitamin K compared to Covid-19 patients with a better outcome.
Now vitamin K assists the body in clotting. So you might think that having plenty of vitamin K would increase clotting, thereby increasing the risk of thrombosis (blood clots blocking veins or arteries). But the opposite may well be true. Having normal levels of vitamin K may be beneficial by keeping the blood clotting system in balance. A video by Dr. Mobeen Syed here discusses the benefits of having plenty of vitamin K, so as to avoid Covid-19-related clotting and thrombosis.
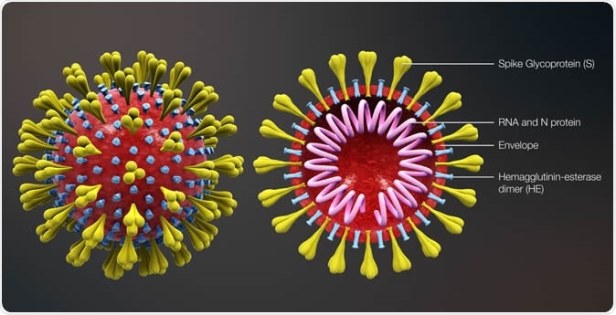
The Spike Glycoprotein
We’ve all see the artist’s conception of the Coronavirus in the media, with colorful idealized Spike proteins all over the spherical virus. The real shape of that Spike is rather convoluted, as it is a protein folded in a complex manner, with many grooves and protrusions. In addition, what those graphics never show you, the Spike is coated with sugar chains, which are very flexible, and serve to fend off the immune system, as they continually moved about [7]. A recent study by Casalino et al. found that these sugar chains protect about 90% of the stalk of the Spike and 62% of the head of the Spike [7].
The protection, though, is against proteins, such as immune system proteins that might recognize the Spike as foreign. Small molecules, such as medications or natural compounds, functioning as inhibitors, are small enough to reach to the Spike protein, past the sugar chains. In the case of small molecule inhibitors, the sugars protect only 26% of the stalk and 20% of the head [7]. The take away is that inhibitors (e.g. quercetin, EGCG, curcumin) may be better at attacking the SARS-CoV-2 Spike than the proteins of the immune system.
High Altitudes
Finally, this week a new study determined that high altitudes have detrimental effects on persons infected with Covid-19 [8]. Woolcott and Bergman found that men under 65 years and living at altitudes above 2000 meters (6500 feet) are at increased risk of death from Covid-19. There were several metrics from the study. First, the overall death rate in “U.S. counties located at ≥2,000 m elevation vs. those located below 1,500 m” [8] was higher, with almost four times as many deaths per 100,000 of the population. Second, in Mexico, a similar comparison by altitude found only a 36% higher risk of death, and only for those under 65 years of age. Third, in the same altitude comparison, men had a 31% higher risk of death at the higher altitude [8].
The proposed reason for this increase in mortality is the lower amount of oxygen in the air at higher altitudes. This may make it even more difficult to breathe when combined with a severe case of Covid-19. Then men are more likely to have a severe case than women. But this explanation is not very convincing. It doesn’t explain why the difference in mortality was found only for those under 65 years, when most of the severe cases are in the elderly, over 65 years. It also does not explain the gender difference very well. Yes, more men have severe cases, but there should have been some effect in women, if the reason is only the lower oxygen content in the air. So it remains unclear whey altitude affects Covid-19 mortality.
Ronald L. Conte Jr.
Covid.us.org
Note: the author of this article is not a doctor, nurse, or healthcare provider.
1. Sajadi, Mohammad M., et al. “Temperature, Humidity, and Latitude Analysis to Estimate Potential Spread and Seasonality of Coronavirus Disease 2019 (COVID-19).” JAMA Network Open 3.6 (2020): e2011834-e2011834.
2. Edridge, Arthur WD, et al. “Human coronavirus reinfection dynamics: lessons for SARS-CoV-2.” medRxiv (2020).
3. Meltzer, David O., et al. “Association of Vitamin D Deficiency and Treatment with COVID-19 Incidence.” medRxiv (2020).
4. Grant, William B., et al. “Evidence that vitamin D supplementation could reduce risk of influenza and COVID-19 infections and deaths.” Nutrients 12.4 (2020): 988.
5. Klok, Frederikus A., et al. “Confirmation of the high cumulative incidence of thrombotic complications in critically ill ICU patients with COVID-19: an updated analysis.” Thrombosis research (2020).
6. Dofferhoff, Anton SM, et al. “Reduced Vitamin K Status as A Potentially Modifiable Prognostic Risk Factor in COVID-19.” Preprints (2020).
7. Casalino, Lorenzo, et al. “Shielding and Beyond: The Roles of Glycans in SARS-CoV-2 Spike Protein.” bioRxiv (2020).
8. Woolcott, Orison O., and Richard N. Bergman. “Mortality Attributed to COVID-19 in High-Altitude Populations.” medRxiv (2020).